Continued from Part 21
On the morning after we returned from the trip to Duke, we were awakened by an early morning phone call. It was a nurse from the nursing home where my grandmother was, calling to tell us that Grandmom had taken a turn for the worse. My siblings and I quickly got dressed and raced to the nursing home.
Grandmom looked and sounded awful. She was unresponsive and was struggling so much to breathe that the nurse was having to suction the secretions in her throat every 30 minutes or more to help her breathe. Grandmom had nursing support both from her nursing home and from a Hospice service, and the Hospice advised us to just sit with her and talk to her. “She hasn’t been able to eat or drink in a couple of days, and she has a high fever that isn’t responding to medication. We are giving her medicine to keep her comfortable,” she told us.
So that’s what we did; we sat with Grandmom, with one of us holding each of her hands, and we talked to her. We told her that we loved her and that we were so very proud of her. We remembered aloud some of the good times we’d had with her, and we told her that Granddad, her husband of 50 years, was waiting for her in heaven. She didn’t seem to be in pain, really, but she didn’t seem very comfortable either. I hated seeing her like that; she had suffered so much already as a result of the decline in her physical and mental status over the past couple of years. She had worked hard in her 90 years of life and had fought hard since she’d gotten sick. The hospice nurse told us that she thought Grandmom would only be able to hang on for a few more days. We brushed her hair back out of her face and cried quiet tears as we sat with her, trying to figure out what we could do to help her.
As the hospice nurse got up to leave, I stepped into the hallway and told her that I did NOT want Dad to be told about Grandmom’s worsened condition, nor did I want anything about Dad’s illness to be mentioned in Grandmom’s presence. From my perspective, each of them had enough to cope with at the time; I felt it was our responsibility to take care of them and to protect them so that neither of them would have to worry about the other one at that point. The hospice nurse made it obvious that she disagreed with me; she even said that she planned to “stop by” my parents’ house later that day to “check in.” Hmmm.
First of all, how freaking RUDE is it to “stop by” the house of someone who is very ill? Secondly, it was obvious by her refusal to commit to keeping quiet that it was a fair bet that she was at least considering telling Dad about his mother’s condition. I didn’t have any official authority about anything that was going on with either my dad or my grandmother, but I had been very involved in caring for both of them, and here was a fact to which Buttinsky Nurse evidently had yet to be enlightened: My mother, my siblings, and I were operating as a team. There was no division of power or usurping the authority of one of us by going behind that person’s back to confer with (or tattle to) another one. That Daughter Bear (and Granddaughter Bear) instinct was kicked into high gear. I left it with B. Nurse (ok, I had another “B-word” nickname for her in my head besides “Buttinsky”) that she was to check with my mom, who did have legal authority in both cases, before she did anything, including “stopping by” my parents’ house.
Meanwhile, back at my parents’ house, Dad wasn’t feeling better as we’d been told that he would be after the Avastin infusion a couple of days before; in fact, he had developed a severely sore throat and his headache and fatigue seemed to be worsening. He was struggling just to sit in his recliner in the den while the grandchildren waited on him and some Christmas decorations were being put up in my parents’ house. A flurry of phone calls and text messages went around and it was decided that we would divide up to spend as much time as we could with Grandmom, to help take care of Dad, and to function as the support staff to get food and whatever else was needed for those in the first two positions.
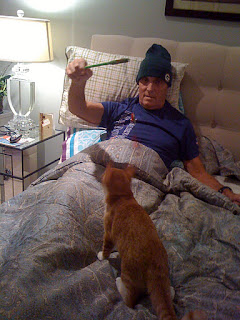 |
| Dad, with his Healing Hat on, playing with Foster |
All in all, Dad felt like crap. As usual, he was trying his best to “hang tough,” attempting to distract himself by playing with his cat Foster and to keep a smile on his face, especially around his six grandchildren. Not even chocolate ice cream, tomato soup (his favorite), or a Diet Coke from Sonic made him feel any better at all, though. In what became a very unfortunate and tragic pattern for us over the next six weeks, doctors’ offices were closed that day due to the holiday, and so we knew we wouldn’t be able to get in touch with the oncologist who was familiar with Dad and his case. By the end of the day, I had decided to call the emergency line at the neuro-oncologists’ office at Duke to let them know about the new/worsening symptoms and the lack of improvement. The on-call doctor called me back fairly quickly, listened to my concerns, and then said that the problematic symptoms were likely just a side effect of the chemo and/or the Avastin and that we should increase Dad’s pain medications and check with the hometown oncologist on Monday morning. I felt like I was trying to move a mountain, one spoonful of dirt at a time.


No comments:
Post a Comment